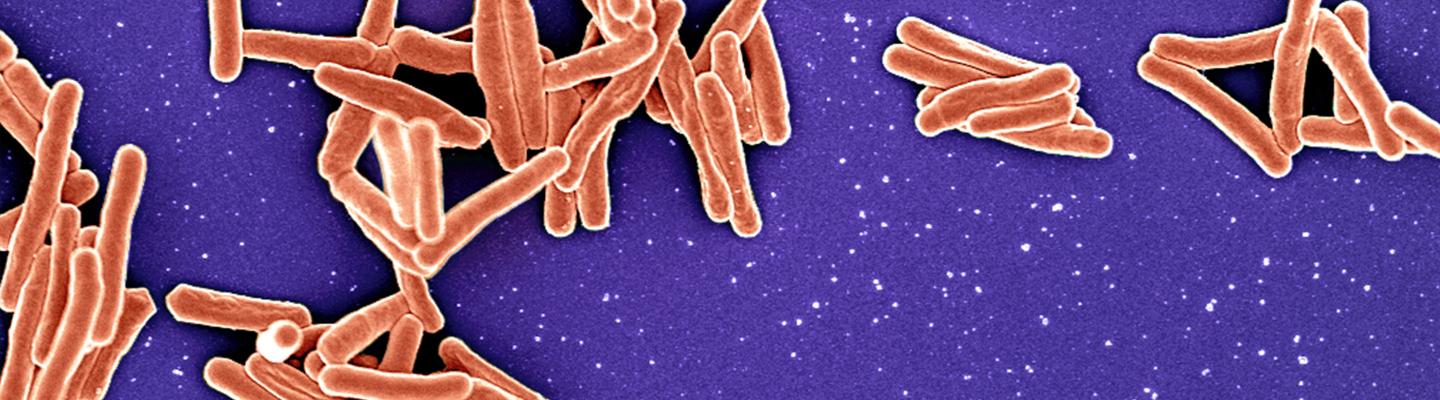
Tuberculosis (TB) is a contagious disease caused by infection with Mycobacterium tuberculosis (Mtb) bacteria. It is spread through the air when a person with TB disease of the lungs or throat coughs, speaks or sings, and people nearby breathe in these bacteria and become infected.
TB typically affects the lungs, but it can also affect other parts of the body, including the kidney, spine and brain. Not everyone infected with TB bacteria becomes sick. People who have latent TB infection have the TB bacteria in their bodies but are not sick and cannot spread the bacteria to others. Individuals with active TB disease, however, are sick and may also be able to transmit the bacteria to others. Many people with latent TB never develop active TB disease. For people with weakened immune systems, such as those living with HIV infection, the risk of developing TB disease is much higher than for those with normal immune systems. Both latent TB infection and active TB disease can be treated. Without treatment, latent TB infection can progress to TB disease, and without proper treatment, TB disease can kill.
Why Is the Study of Tuberculosis a Priority for NIAID?
Tuberculosis is the leading infectious cause of death worldwide. In 2017, 10 million people became ill with TB, and 1.6 million people died of TB disease including 230,000 children, according to the World Health Organization. Over the past 200 years, TB has claimed the lives of more than one billion people---more deaths than from malaria, influenza, smallpox, HIV/AIDS, cholera, and plague combined. Although TB treatment exists, drug resistance is a continued threat.
How Is NIAID Addressing This Critical Topic?
NIAID supports and conducts basic, translational and clinical research to better understand TB and expedite the development of innovative new tools and strategies to improve diagnosis, prevention and treatment of TB.
Highlights

NIAID Strategic Plan for Tuberculosis Research, 2024 Update
Tuberculosis is the second leading infectious cause of death worldwide. In the updated strategic plan, NIAID details four strategic priorities that are critical to the development and evaluation of the knowledge and tools needed to end TB globally.
NIH Clinical Trial of Tuberculous Meningitis Drug Regimen Begins
A trial of a new drug regimen to treat tuberculous meningitis (TBM) has started enrolling adults and adolescents in several countries where tuberculosis (TB) is prevalent.
News Releases
NIAID Now Blog
Funded Research News
- Study Challenges Assumptions About How Tuberculosis Bacteria Grow
November 15, 2024 - Uncovering Molecular Pathways
November 7, 2024 - Reviving Immune Responsiveness after Tuberculosis
October 10, 2024
Related Public Health and Government Information
To learn about risk factors for tuberculosis and current prevention and treatment strategies visit the MedlinePlus tuberculosis site.