January 5, 2021
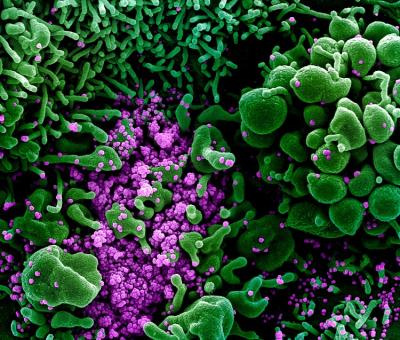
A colorized scanning electron micrograph of an apoptotic cell (green) heavily infected with SARS-CoV-2 virus particles (purple), isolated from a patient.
A Phase 2/3 clinical trial has begun to evaluate a combination investigational monoclonal antibody therapy for its safety and efficacy in people who have mild or moderate COVID-19. The two experimental antibodies, BRII-196 and BRII-198, target SARS-CoV-2, the virus that causes COVID-19. The trial, known as ACTIV-2, is sponsored by the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health.
NIH’s Accelerating COVID-19 Therapeutic Interventions and Vaccines (ACTIV) program is a public-private partnership to develop a coordinated research strategy for speeding development of the most promising treatments and vaccine candidates. ACTIV-2 is a master protocol designed for evaluating multiple investigational agents compared to placebo in adults with mild-to-moderate COVID-19. The trial, led by the NIAID-funded Advancing Clinical Therapeutics Globally for HIV/AIDS and Other Infections (ACTG) and supported by PPD (Wilmington, N.C.), will enroll participants at sites around the world.
The ACTIV-2 study began on August 4, 2020, with an evaluation of LY-CoV555, an investigational monoclonal antibody discovered by AbCellera Biologics (Vancouver, British Columbia) in collaboration with NIAID’s Vaccine Research Center. LY-CoV555 was developed further and manufactured by Eli Lilly and Company (Indianapolis, Indiana), in partnership with AbCellera. On November 10, 2020, LY-CoV555, also known as bamlanivimab, was granted Emergency Use Authorization by the U.S. Food and Drug Administration (FDA) for treating mild-to-moderate COVID-19 in adults and children over 12 years old who are at high risk for progressing to severe COVID-19 and/or hospitalization. With the initiation of the BRII-196 and BRII-198 experimental monoclonal antibodies in the ACTIV-2 study, the LY-COV555 sub-study will close to enrollment.
BRII-196 and BRII-198 are investigational, neutralizing monoclonal antibodies manufactured by Brii Biosciences (Durham, N.C., and Beijing). Antibodies are infection-fighting proteins naturally made by the immune system that can bind to viruses and prevent them from infecting cells. BRII-196 and BRII-198 are synthetic versions of antibodies produced naturally by humans. Data on each antibody from Phase I trials that are currently ongoing support the doses being used in the ACTIV-2 trial.
The ACTIV-2 study design allows researchers to observe the therapeutics’ efficacy in a small group of volunteers and then administer it to a larger group if the antibody appears safe and effective. The trial will initially enroll 220 participants with mild or moderate COVID-19, who are at risk for disease progression. Half of the participants (110) will receive BRII-196 and BRII-198 through intravenous infusions, while the remaining half will receive placebo infusions. Participants are assigned at random to one of the treatment groups, and the trial is blinded so neither participants nor investigators will know who is receiving the antibody therapy. Participants will attend a series of clinic or at-home visits by clinicians to track their condition and will be followed for a total of 72 weeks.
An independent Data and Safety Monitoring Board (DSMB) overseeing the trial will review the data collected at 28 days. They will monitor data to see if the therapy is safe, can reduce the duration of COVID-19 symptoms and can eliminate the presence of viral RNA in the body. If there are no serious safety concerns and the results seem promising, the trial will transition to Phase 3 to enroll approximately 622 additional outpatient volunteers, for a total of 842 trial participants. These new participants will be randomized to receive the therapeutic or a placebo.
The primary objective of the Phase 3 trial is to determine if the therapy prevents either hospitalization or death by 28 days after study entry.
The study team for ACTIV-2 is led by protocol chairs Kara W. Chew, M.D., M.S., of the University of California, Los Angeles (UCLA), and Davey Smith, M.D., MAS, of the University of California, San Diego. Eric S. Daar, M.D., of UCLA, and David Wohl, M.D., of the University of North Carolina at Chapel Hill (UNC), serve as protocol vice-chairs. The ACTG network is led by chair Judith Currier, M.D. (UCLA) and vice-chair Joseph Eron, M.D., of UNC. The study of BRII-196 and BRII-198 is led by Eric S. Daar, M.D., of the Harbor-UCLA Medical Center and Teresa H. Evering, M.D., M.S., of Weill Cornell Medical Center.
For more information on this study, please visit www.riseabovecovid.org, or visit ClinicalTrials.gov and search identifier NCT04518410.
Contact
To schedule interviews, contact:
Elizabeth Deatrick
301-402-1663
NIAIDNews@niaid.nih.gov

