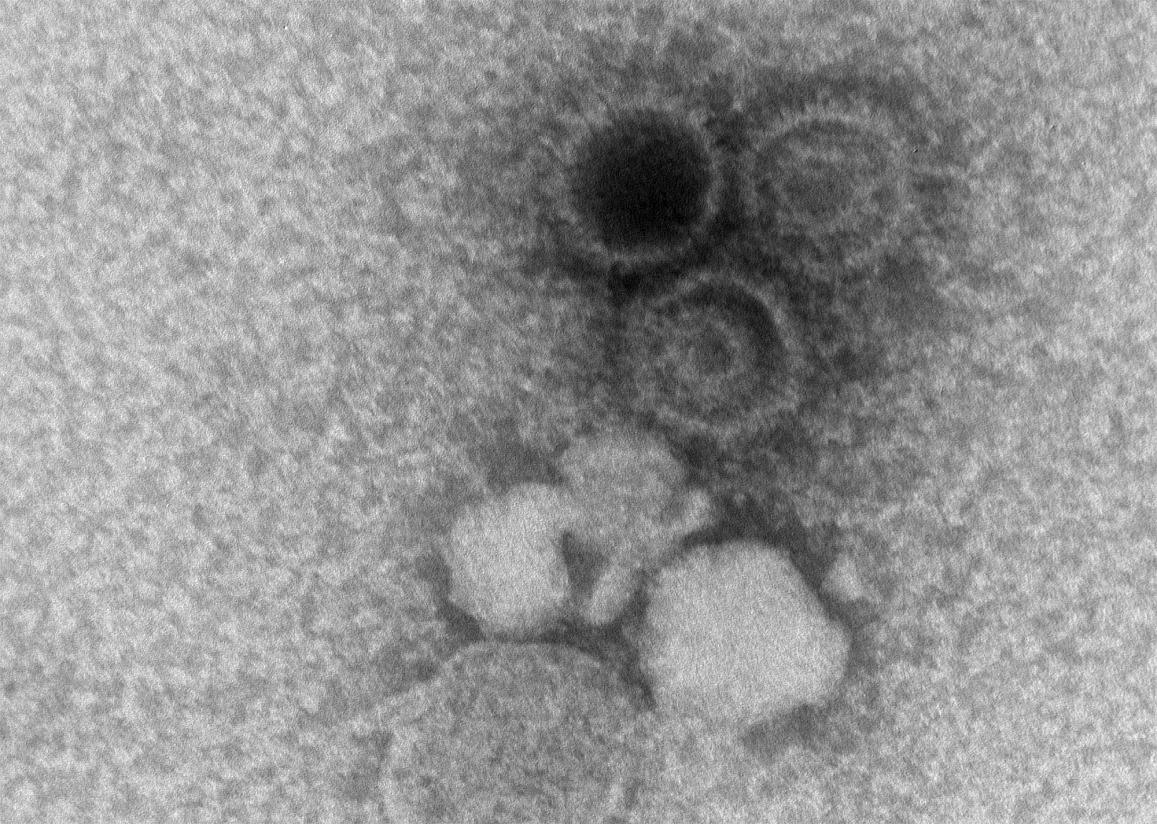
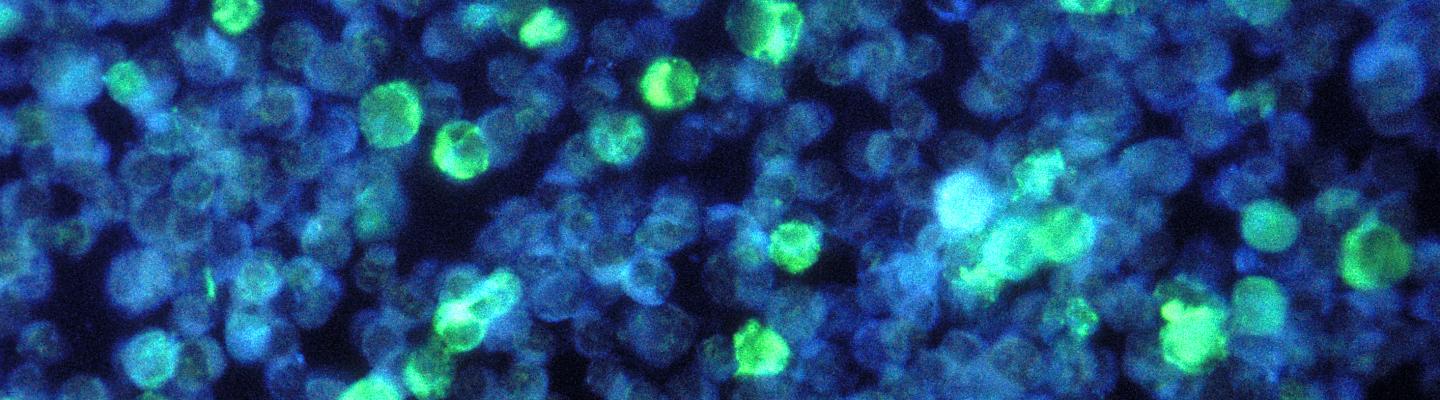
XLP, which primarily affects boys, is characterized by a life-long vulnerability to Epstein-Barr virus (EBV), a common type of herpes virus. This virus usually does not cause symptoms other than a brief infection or mononucleosis, but people with XLP can have severe reactions to EBV infections.
XLP is caused by mutations in a gene called SH2D1A, which is located on the X chromosome and provides instructions for making SAP protein. These mutations can alter the structure and function of SAP or the amount of SAP produced. Lack of functional SAP causes defects in T- and B-cell interactions, which leads to abnormal immune responses to EBV.
People with XLP are healthy until they are exposed to EBV. Then, they can become seriously ill and experience swollen lymph nodes, an enlarged liver and spleen, hepatitis and lymphoma. Some people with XLP have developed lymphoma in the absence of EBV infection.
XLP may be suspected based on an overactive immune response to viral infection, such as development of severe mononucleosis in response to EBV infection. A blood test showing low antibody, or immunoglobulin, levels also may suggest XLP. Diagnosis of the disease requires a demonstrated lack of functional SAP or identification of a loss-of-function mutation in the SH2D1A gene.
Evidence suggests that rituximab, a drug that targets B cells, can be life-saving in people with XLP and severe mononucleosis caused by EBV. Doctors may use immunoglobulin replacement therapy to treat the low level of antibodies that occurs in some patients with XLP, but this will not necessarily protect against EBV infection. Bone marrow or umbilical cord blood transplantation, which re-set and replenish the immune system, can effectively cure XLP.
Related Scientific Advances
NIH Scientists Find Weak Points on Epstein-Barr Virus
March 12, 2024Studies of interactions between two lab-generated monoclonal antibodies (mAbs) and an essential Epstein-Barr virus (EBV) protein have uncovered targets that could be exploited in designing treatments and vaccines for this extremely common virus. The research was led by Jeffrey I. Cohen, M.D., and colleagues from NIAID.
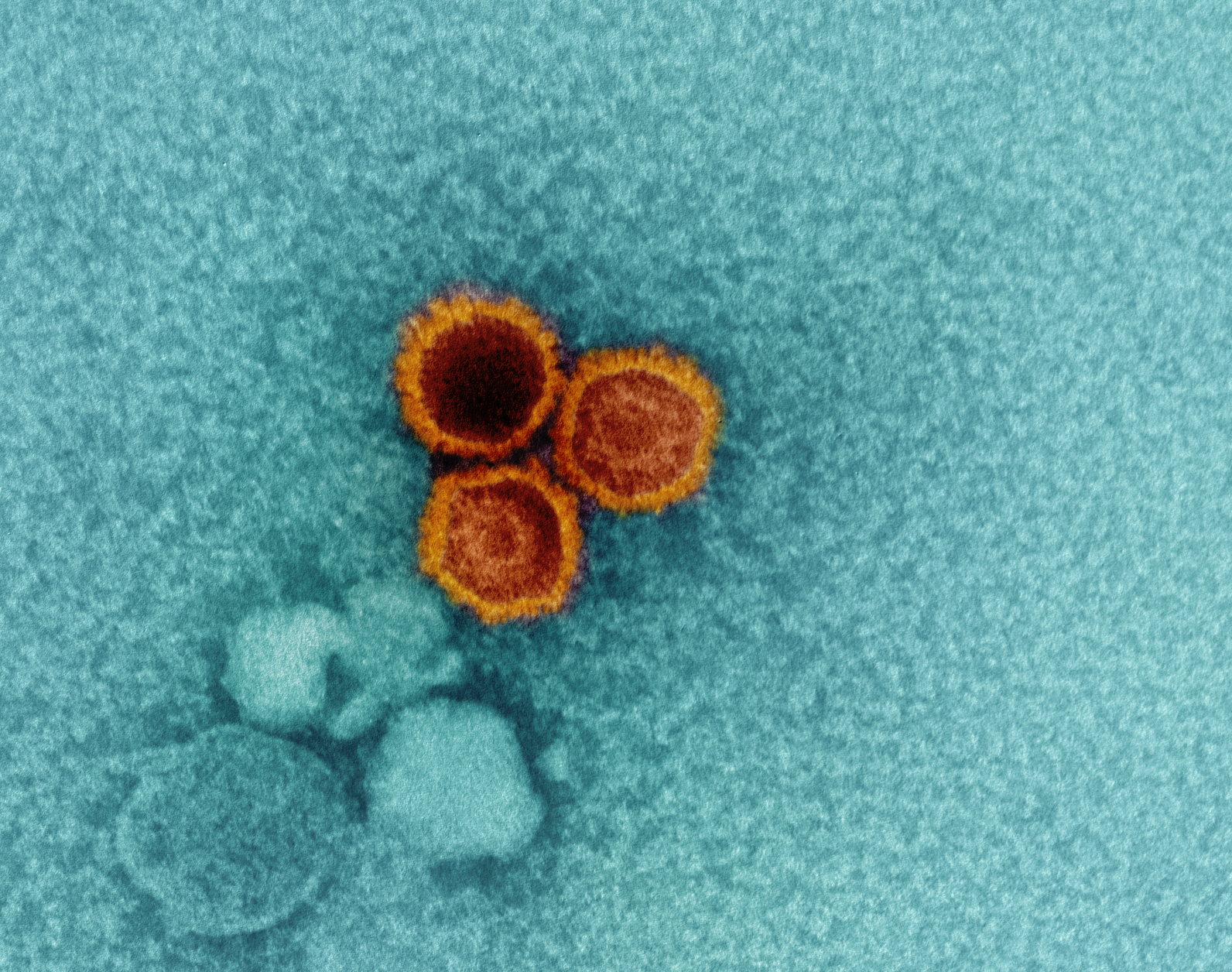
Experimental Monoclonal Antibodies Show Promise Against Epstein-Barr Virus
October 27, 2022A panel of investigational monoclonal antibodies (mAbs) targeting different sites of the Epstein-Barr virus (EBV) blocked infection when tested in human cells in a laboratory setting. Moreover, one of the experimental mAbs provided nearly complete protection against EBV infection and lymphoma when tested in mice. The results appear online in the journal Immunity.