Chronic granulomatous disease (CGD) is a genetic disorder in which white blood cells called phagocytes are unable to kill certain types of bacteria and fungi. People with CGD are highly susceptible to frequent and sometimes life-threatening bacterial and fungal infections.
What Is Chronic Granulomatous Disease?
Causes
CGD is caused by defects in an enzyme, NADPH oxidase, that phagocytes need to kill certain bacteria and fungi. Mutations in one of five different genes can cause these defects.
Symptoms & Diagnosis
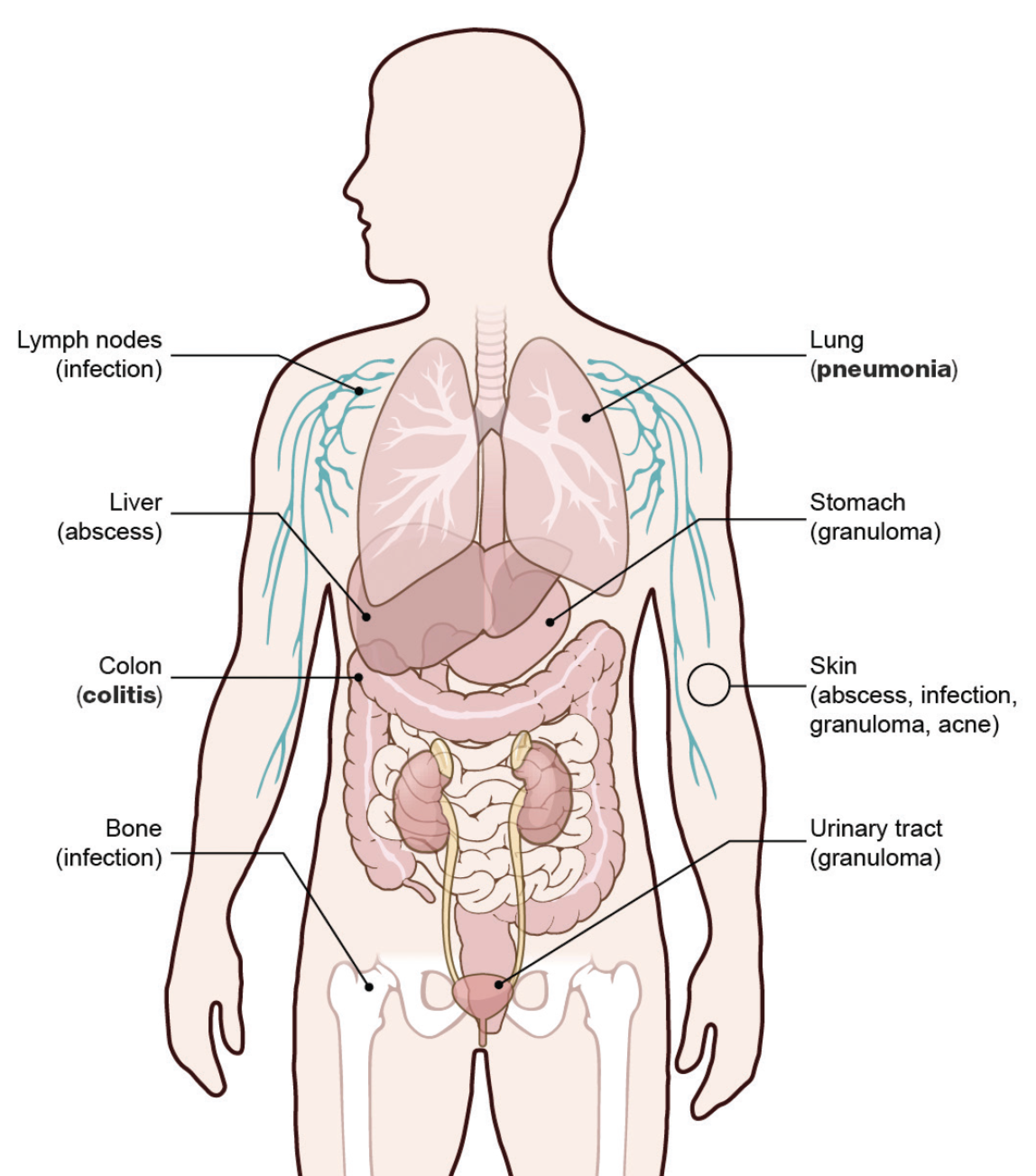
People with CGD are highly susceptible to infections caused by certain bacteria and fungi, such as Staphylococcus aureus, Serratia marcescens, Burkholderia cepacia, Nocardia species, and Aspergillus species. These people may develop abscesses (boils) in their lungs, liver, spleen, bones, or skin; and masses of cells, called granulomas, that can obstruct the bowel or urinary tract. In some people, granulomas can cause an inflammatory bowel disease similar to Crohn’s Disease. In addition, heart or kidney problems, diabetes, and autoimmune disease may occur in people with CGD, but this varies depending on which gene is mutated.
CGD is diagnosed by special blood tests that show how well phagocytes produce hydrogen peroxide, an indicator that they are functioning properly.
Treatment
People with CGD take lifelong regimens of antibiotics and antifungals to prevent infections. Injections with interferon gamma, a protein that improves the activity of phagocytes, also may help reduce the number of severe infections. Abscesses need aggressive care that may include surgery. Granulomas may require steroid therapy. Some people with CGD have been treated successfully with bone marrow transplantation.
NIAID scientists are exploring gene therapy approaches to address the underlying genetic defects that cause CGD. In early 2017, they described using the CRISPR-Cas9 gene-editing strategy to correct the defective gene in cells taken from patients with the X-linked form of CGD.
NIAID also supports the development of antifungal drugs and other therapies to curb infections and improve outcomes for people with CGD.
Medications