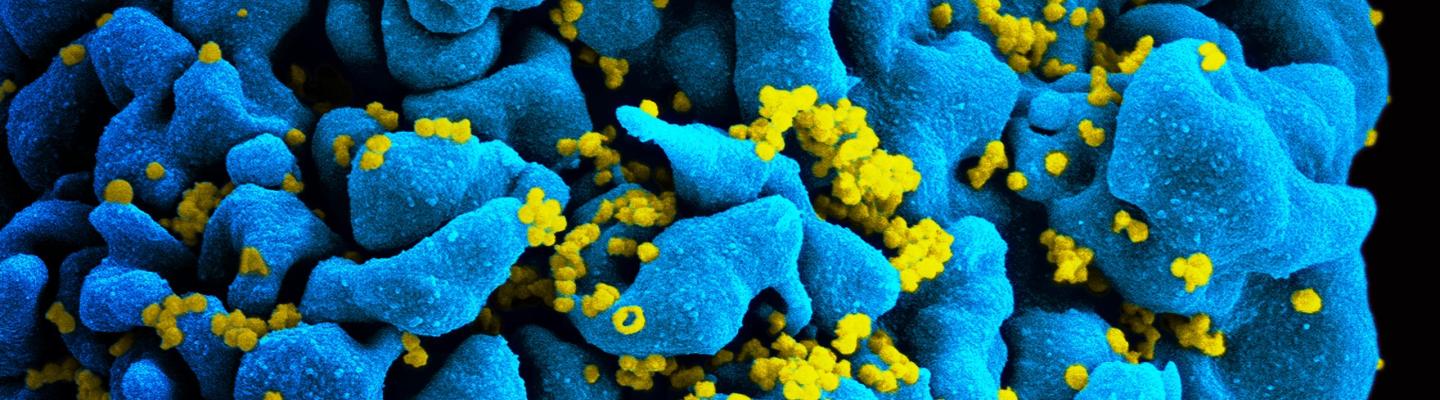
This approach to developing an HIV vaccine is based on theory and involves establishing an understanding of the immune response to HIV infection and finding ways to generate and enhance that response through vaccination. Some strategies aim to prevent HIV infection via antibodies, while others strive to generate a protective cellular response.
Designing an Antibody-Based HIV Vaccine
No one with HIV has ever developed an immune response that cleared the infection, so scientists do not yet know what constitutes an effective immune response to the virus. However, researchers have observed that some people living with HIV naturally develop broadly neutralizing antibodies (bNAbs) against the virus after months or years of infection. These bNAbs have been shown in the laboratory to stop most HIV strains from infecting human cells. They do not eradicate the virus from people living with HIV, however, because by the time a bNAb appears in a mature form, HIV has proliferated and mutated to escape neutralization by that antibody. But if a vaccine could generate bNAbs in healthy people before exposure to HIV, the antibodies potentially could fight the virus off completely.
Numerous studies by NIAID scientists, grantees and others have provided evidence that a vaccine eliciting bNAbs might protect people from HIV. First, researchers have shown that infusing bNAbs into monkeys protects them from infection by a human-monkey hybrid virus similar to HIV. Second, clinical studies have demonstrated that infusing bNAbs into people living with HIV reduces the amount of virus circulating in their blood. Third, laboratory studies have shown that bNAbs markedly suppress HIV production from infected immune cells where the virus hides in the body.
To directly test the hypothesis that bNAbs can prevent HIV infection, a pair of large, multinational, NIAID-funded clinical trials launched in spring 2016, called the AMP (antibody-mediated prevention) Studies, are giving intravenous infusions of bNAbs to healthy adults at high risk for HIV to see if that protects them from the virus.
One of the first potent bNAbs to be discovered, VRC01, was identified and isolated by scientists at the NIAID Vaccine Research Center (VRC) in 2010. Since that time, researchers have isolated hundreds of other bNAbs, and many scientists have embarked on projects to reverse-engineer an HIV vaccine that elicits one of these antibodies. The basic process involves identifying the site where a bNAb binds to the virus, characterizing the molecular structure of that site in detail, designing a protein replica of the binding site, and testing the replica, called an immunogen, in animals and people to see if it elicits the desired bNAb.
In 2018, VRC scientists reported that a vaccine based on the fusion peptide—a vulnerable site on HIV that helps the virus fuse with a cell to infect it—elicited neutralizing antibodies in mice, guinea pigs and monkeys. VRC scientists first identified the fusion peptide target in 2016 and consider it particularly promising for use as a vaccine because its sequence is the same across most strains of HIV, it is exposed on the spike on HIV’s surface, it lacks the sugars that obscure the immune system’s view of other sites on the virus’ outer shell, and the immune system makes a strong response to it. The experimental vaccine includes a portion of the fusion peptide bonded to a carrier that evokes a strong immune response. This immunogen is paired with a replica of the spike on HIV’s surface. The scientists are working to optimize the vaccine and ultimately aim to manufacture a version of it suitable for safety testing in human volunteers in a carefully designed and monitored clinical trial.
One of the signature characteristics of powerful HIV bNAbs is that they mutate dozens of times before achieving their mature HIV-fighting form. This means eliciting such antibodies through vaccination likely would involve an initial vaccine to kick-start bNAb development followed by a series of vaccinations to coax the bNAb along the desired developmental pathway. A 2011 VRC-led study of antibody genetics enabled scientists to deduce the step-by-step evolution of VRC01 and related antibodies. Moreover, studies by VRC scientists and NIAID grantees have revealed how bNAbs and HIV stimulate each other to evolve, shedding light on the necessary structures of the initial and intermediate immunogens of an HIV vaccine regimen that would generate a nascent bNAb and coax it to mature. A 2015 trio of animal studies by NIAID grantees provided evidence that such a strategy could generate the desired antibody response.
A related approach to creating an HIV vaccine is to elicit a variety of HIV antibodies, each of which neutralizes only a modest variety of HIV strains but together neutralize a wide range. This strategy is attractive because some modestly neutralizing antibodies have a much shorter developmental pathway than bNAbs, thus requiring far fewer immunogens.
Understanding HIV Structure
BNAbs bind mainly to five unchanging sites located on spikes on HIV’s surface. These spikes are known as the envelope glycoprotein, or Env. Each spike is composed of three identical pairs of proteins, collectively called the trimer. Many attempts to immunize against HIV used just one segment of the trimer, yielding suboptimal results. Eventually it became clear that the whole trimer would be a more effective immunogen. However, Env is extremely difficult to stabilize as a stand-alone molecule separate from HIV. So it was a major advance when, in 2013, NIAID grantees engineered a more stable form of Env and obtained an atomic-level image of it.
The following year, a study co-led by NIH scientists discovered that an HIV vaccine that teaches the immune system to neutralize the virus should be based on the configuration Env takes before it fuses with a cell. VRC researchers produced a high-resolution structural model of this pre-fusion viral spike, a valuable tool for HIV immunogen design. Further studies by NIAID grantees have demonstrated that it is possible to immunize animals with HIV trimer proteins and to modify Env immunogens so they stimulate production of the earliest precursors of particular bNAbs. Such experimental structure-based vaccines currently are being evaluated in early-stage clinical trials at NIAID and elsewhere.
Structural studies by VRC scientists led to the 2016 discovery of the fusion peptide as a vaccine target. The scientists characterized in atomic-level detail how a bNAb isolated from the blood of a person living with HIV binds to the fusion peptide and stops the virus from infecting a cell. These insights led to the development of a fusion peptide-based vaccine that can elicit neutralizing antibodies in animal models.
Designing a Cell-Based HIV Vaccine
An alternative theoretical approach to HIV vaccine design aims to elicit a potent cell-based immune response, rather than an antibody response. Some NIAID grantees pursuing this strategy aim to elicit cellular immune responses to the most static regions of HIV’s proteins by creating vaccine components focused solely on these regions. In contrast, other grantees strive to elicit cellular immune responses using so-called mosaic antigens, which are computationally derived proteins created by stitching together genetic sequences from across the whole HIV genome.
Taking a different tack, another NIAID grantee pursuing a cell-based response to HIV created an immunogen by placing selected HIV genes into an unrelated virus called cytomegalovirus (CMV). Most people naturally acquire CMV, which usually does not cause any symptoms in healthy adults, and which persists in the body at very low levels yet garners a large immune response, as T-cells armed to fight the virus circulate in high numbers in the blood. In a preliminary test of this approach, monkeys infected with SIV, the simian form of HIV, were vaccinated with a monkey version of the CMV immunogen. More than half of the vaccinated animals completely controlled SIV and ultimately eliminated it from their bodies within a year or two, marking the first time an immune response cleared an AIDS-causing virus. Scientists are still investigating how this vaccine works at the cellular and molecular levels, and clinical trials are awaiting the selection and manufacture of a final vaccine candidate.