Epithelial Therapeutics Unit
Ian A. Myles, M.D., M.P.H.
Principal Investigator, Epithelial Therapeutics Unit
Chief Medical Research Officer, U.S. Public Health Service Commissioned Corps
Contact: ian.myles@nih.gov
Specialty(s): Allergy and Immunology, Internal Medicine Provides direct clinical care to patients at NIH Clinical Center

Highlights
NIAID Discovery Leads to Novel Probiotic for Eczema
June 26, 2024
NIAID research has led to the availability of a new over-the-counter topical eczema probiotic. The probiotic is based on the discovery that bacteria present on healthy skin called Roseomonas mucosa can safely relieve eczema symptoms in adults and children.
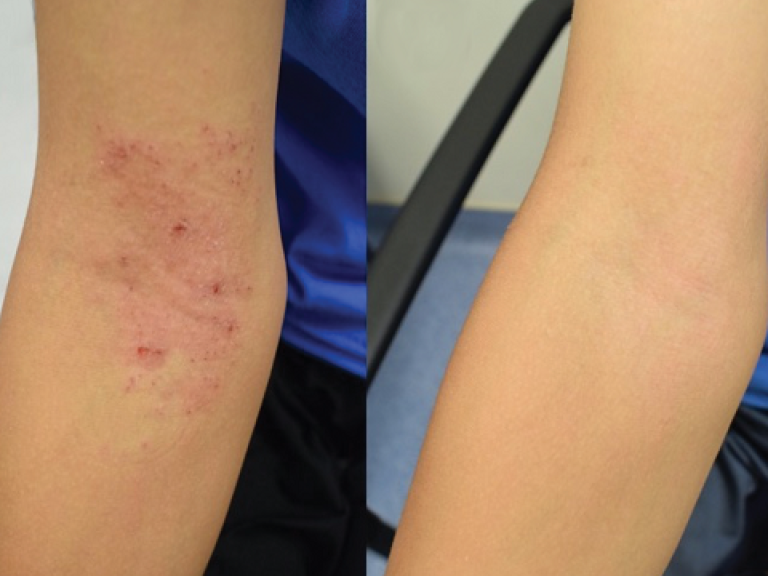
Probiotic Skin Therapy Improves Eczema in Children, NIH Study Suggests
September 9, 2020
An experimental treatment for eczema safely reduced disease severity and increased quality of life for children as young as 3 years old, NIH study shows.
Major Areas of Research
- Therapeutic effects of microbiome manipulation in the treatment of eczema (atopic dermatitis)
- Role of the microbiome during the normal processes of tissue repair and wound healing
- Mechanisms of susceptibility to epithelial infections with Staphylococcus aureus
- Dietary influences on immune development
- Role of environmental exposures in creating dysbiosis
Program Description
Our group focuses on how human health is affected by the normal microorganisms that live on our skin (collectively termed the microbiome). Our emphasis is on eczema (also called atopic dermatitis or AD), which is an inflammatory disease of the skin associated with reduced quality of life and high risk of developing asthma, allergic rhinitis, and food allergies. AD afflicts 5 to 25 percent of children globally and has a reported prevalence of 8 to 18 percent in the United States. Patients with AD require increased health care utilization, suffering substantially greater out-of-pocket costs than matched controls. The underlying pathology of AD includes defective skin barrier function, susceptibility to Staphylococcus aureus skin infection, and immune dysregulation. Current therapeutic options are limited by their requirement for multiple-times-per-day applications and/or substantial cost. While the natural history of AD suggests that 50 to 90 percent of patents will self-resolve by approximately 10 to 15 years of age, the prolonged barrier defects may put patients at risk for development of associated allergic diseases.
Recent work has uncovered that the skin microbiome is significantly different between healthy controls and patients with AD and that early commensal diversity may protect against development of AD. These realizations suggest that the skin microbiome contributes to AD presentation through both harmful and protective pathways. Our group identified a species of bacteria from normal healthy skin, called Roseomonas mucosa, which showed promising features in cell culture and mouse models that suggested the bacteria might be able to treat patients with eczema. We have since transitioned into a clinical trial using Roseomonas mucosa as a topical treatment for eczema. While guided by the science, our group strives to find treatments that not only improve symptoms but also provide relief without worsening the financial and/or time burdens that disease places on patients and their families.
Beyond the immediate clinical trial, our group is interested in the role the microbiome plays in normal tissue repair and wound healing. The skin, the colon, and the lungs all have to ‘renew’ themselves naturally due to normal day-to-day wear-and-tear. These tissues cannot correctly do so without contact with various microorganisms, and we endeavor to better understand why. Furthermore, we are interested in how environmental factors can influence health through effects on the microbiome. For example, we are interested in uncovering how a healthy diet encourages the types of microorganisms that support good health. This includes not only dietary fats and sugars, but also early exposures like breast milk. We also work to uncover what chemical exposures (such as soaps or topical preservatives) may benefit or harm the microbial balance in ways that influence health and disease.
Collaboration Interests
Breast milk has numerous well-known benefits for the offspring’s immune system; however, many of the mechanisms of these effects are unknown. ETU is interested in one specific finding that early breast milk (such as colostrum) is enriched for a specific type of T cell known as an effector memory CD8+ T cell. Our work in mice and cell culture has established that these cells can transfer immune responses – i.e., people who are unable to react to certain pathogens can be made reactive when treated with byproducts of these cells. Therefore, we seek to identify the exact mechanism by which these T cells impart cellular memory to the offspring and hope to synthesize treatments based on this natural process.
Parties interested in pursuing collaborative research in the research areas above should reach out to Dr. Ian Myles.
Biography
Education
B.S., 2001, Colorado State University, Fort Collins, CO
M.D., 2005, University of Colorado, Boulder CO
M.P.H., 2016, George Washington University, Washington, DC
Dr. Myles was born and raised in Colorado. He graduated with a B.S. in biology from Colorado State University in 2001 and then obtained an M.D. from the University of Colorado in 2005. He completed an internal medicine residency at The Ohio State University prior to beginning fellowship training in allergy and clinical immunology at NIH. He worked under the mentorship of Dr. Sandip Datta investigating the mechanistic details of susceptibility to S. aureus skin infections. In 2011, Dr. Myles became a commissioned officer in the United States Public Health Service Commissioned Corps. LCDR Myles has supported several USPHS missions, from the Ebola virus vaccine trial in West Africa to congressional Gold Medal Ceremonies at the U.S. Capitol. In 2013, he was awarded a position as an assistant clinical investigator in the NIAID Transition Program in Clinical Research. Dr. Myles received his M.P.H. from George Washington University in 2016. In 2018, Dr. Myles became the head of the newly formed Epithelial Therapeutics Unit to evaluate the efficacy and safety of a topical, live bacterial treatment for atopic dermatitis (eczema). He is currently a participant in the Lasker Clinical Research Scholars and Distinguished Scholars programs.
Clinical Studies
Selected Publications
Myles IA, Earland NJ, Anderson ED, Moore IN, Kieh MD, Williams KW, Saleem A, Fontecilla NM, Welch PA, Darnell DA, Barnhart LA, Sun AA, Uzel G, Datta SK. First-in-human topical microbiome transplantation with Roseomonas mucosa for atopic dermatitis. JCI Insight. 2018 May 3;3(9).
Myles IA, Anderson ED, Earland NJ, Zarember KA, Sastalla I, Williams KW, Gough P, Moore IN, Ganesan S, Fowler CJ, Laurence A, Garofalo M, Kuhns DB, Kieh MD, Saleem A, Welch PA, Darnell DA, Gallin JI, Freeman AF, Holland SM, Datta SK. TNF overproduction impairs epithelial staphylococcal response in hyper IgE syndrome. J Clin Invest. 2018 Aug 1;128(8):3595-3604.
Myles IA, Williams KW, Reckhow JD, Jammeh ML, Pincus NB, Sastalla I, Saleem D, Stone KD, Datta SK. Transplantation of human skin microbiota in models of atopic dermatitis. JCI Insight. 2016 Jul 7;1(10). pii: e86955.
Myles IA, Zhao M, Nardone G, Olano LR, Reckhow JD, Saleem D, Break TJ, Lionakis MS, Myers TG, Gardina PJ, Kirkpatrick CH, Holland SM, Datta SK. CD8+ T cells produce a dialyzable antigen-specific activator of dendritic cells. J Leukoc Biol. 2017 Jan;101(1):307-320.
Myles IA, Fontecilla NM, Valdez PA, Vithayathil PJ, Naik S, Belkaid Y, Ouyang W, Datta SK. Signaling via the IL-20 receptor inhibits cutaneous production of IL-1β and IL-17A to promote infection with methicillin-resistant Staphylococcus aureus. Nat Immunol. 2013 Aug;14(8):804-11.
Myles IA, Fontecilla NM, Janelsins BM, Vithayathil PJ, Segre JA, Datta SK. Parental dietary fat intake alters offspring microbiome and immunity. J Immunol. 2013 Sep 15;191(6):3200-9.
Video of Early Clinical Findings
Watch the video outlining the early findings of our clinical trial using live bacteria in the treatment of eczema.
Research Group
Epithelial Therapeutics Unit – work on the interface of environment, the microbiome, and allergic disease

