Clinical Mycology Section
John E. Bennett, M.D.
Senior Investigator
Specialty(s): Infectious Disease, Internal Medicine Provides direct clinical care to patients at NIH Clinical Center

Major Areas of Research
- Cryptococcosis in previously normal patients
- Idiopathic CD4 lymphocytopenia
- Clinical trials of antifungal agents
Program Description
The Clinical Mycology Section focuses on pathogenesis, diagnosis, treatment, prevention, and epidemiology of mycoses, particularly cryptococcosis and candidiasis.
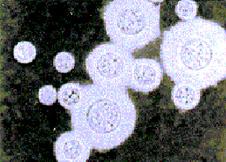
Cryptococcus neoformans var. neoformans: India Ink preparation of cells from a mucoid colony, note the exhuberant capsule.
The incidence of cryptococcosis has risen dramatically in the United States since the onset of the HIV-1 epidemic. Most centers now report that 95 percent of their patients with cryptococcosis are co-infected with HIV-1. Peter Williamson, M.D., Ph.D., and Dr. Bennett are studying previously healthy patients with cryptococcal meningitis to discover underlying predisposing factors and improve therapy. Despite the absence of immunosuppression, these patients are surprisingly difficult to treat compared to those with AIDS and cryptococcosis. A major cause of morbidity and death is cerebral edema and increased intracranial pressure, which usually coexist. Our goals in studying these patients are as follows:
- Understanding the mechanisms causing cerebral edema and increased intracranial pressure
- Searching for genetic markers in the patients and their families that might have predisposed patients to cryptococcosis
- Assessing the role of corticosteroids in controlling cerebral edema
- Evaluating potential new treatments for cryptococcosis
Biography
Education
M.D., The Johns Hopkins University School of Medicine
B.S., Stanford University
Dr. Bennett received his B.S. in chemistry (cum laude) from Stanford University. He earned his M.D. (Alpha Omega Alpha) from The Johns Hopkins University School of Medicine. Dr. Bennett is board-certified in internal medicine and infectious disease. His other honors include master in the American College of Physicians; former president of the Infectious Diseases Society of America; charter president of the Greater Washington Infectious Diseases Society; member of the American Academy of Microbiology, American Society for Clinical Investigation and the American Association of Physicians; co-editor of nine editions of Principles and Practice of Infectious Diseases; and consultant to the Centers for Disease Control and Prevention, American College of Physicians-American Society of Internal Medicine, U.S. Public Health Association, Food and Drug Administration, and U.S. Department of Defense.
Selected Publications
Zonios D, Yamazaki H, Murayama N, Natarajan V, Palmore T, Childs R, Skinner J, Bennett JE. Voriconazole metabolism, toxicity, and the effect of cytochrome P450 2C19 genotype. J Infect Dis. 2014 Jun 15;209(12):1941-8.
Fukuda Y, Tsai HF, Myers TG, Bennett JE. Transcriptional profiling of Candida glabrata during phagocytosis by neutrophils and in the infected mouse spleen. Infect Immun. 2013 Apr;81(4):1325-33.
Bennett JE. Echinocandins for candidemia in adults without neutropenia. N Engl J Med. 2006 Sep 14;355(11):1154-9.
Bennett JE, Izumikawa K, Marr KA. Mechanism of increased fluconazole resistance in Candida glabrata during prophylaxis. Antimicrob Agents Chemother. 2004 May;48(5):1773-7.
Herbrecht R, Denning DW, Patterson TF, Bennett JE, Greene RE, Oestmann JW, Kern WV, Marr KA, Ribaud P, Lortholary O, Sylvester R, Rubin RH, Wingard JR, Stark P, Durand C, Caillot D, Thiel E, Chandrasekar PH, Hodges MR, Schlamm HT, Troke PF, de Pauw B; Invasive Fungal Infections Group of the European Organisation for Research and Treatment of Cancer and the Global Aspergillus Study Group. Voriconazole versus amphotericin B for primary therapy of invasive aspergillosis. N Engl J Med. 2002 Aug 8;347(6):408-15.
Young RC, Bennett JE, Vogel CL, Carbone PP, DeVita VT. Aspergillosis. The spectrum of the disease in 98 patients. Medicine (Baltimore). 1970 Mar;49(2):147-73.
Research Group

Members of the Clinical Mycology Section, August 2013
Training Program
Associate Director of the Infectious Disease Training Program, NIAID

